Gurugram (Haryana) [India], August 1: Policybazaar for Business (PBFB), the corporate arm of one of India’s largest online Insurance platforms, has launched ClaimSetu, a breakthrough AI-powered solution to reduce anxiety/unforeseen situations, simplify, and speed up Group Health Insurance (GHI) reimbursement claims.
While PBFB has already delivered strong claims support to corporate clients with millions of employees, ClaimSetu takes the experience to the next level, giving quantitative scoring like claim insights, approval & scoring around how their claim is expected to be processed. Apart from this is the system, which also helps employees, HR teams, Insurers, and TPAs process claims up to 50% faster with fewer errors and more visibility.
It is currently focused exclusively on streamlining GHI reimbursement claims, a process traditionally burdened by delays due to missing paperwork and a lack of real-time updates. Using cutting-edge Artificial Intelligence (AI), Natural Language Processing (NLP), and Optical Character Recognition (OCR), ClaimSetu reimagines the entire journey, from document submission to final claim approval, making it faster, more accurate, and far more transparent.
“Reimbursement claims remain one of the tedious processes of group health insurance. With ClaimSetu, we are working on where the friction is highest, in GHI reimbursements, and building a system that removes ambiguity and empowers users with real-time updates,” said Sajja Praveen Chowdary, Director, Policybazaar for Business. “This is more than automation; it’s about delivering clarity and trust at the most critical moment of the insurance experience.” Reimagining GHI Reimbursements for Indian Enterprises ClaimSetu is proudly built in India, for Indian enterprises, addressing the unique operational and infrastructural challenges of the country’s corporate health insurance ecosystem. As India’s first homegrown, AI-led claims engine in the B2B insurance space, it marks a leap in digital innovation aligned with the national vision for tech-driven transformation.
Today, many GHI reimbursement claims involve over multiple emails, back-and-forth with TPA or the insurer. ClaimSetu changes this with AI-driven document checks, automated validation, instant alerts, and live tracking via WhatsApp, bringing further speed and clarity to the process.
The platform identifies and extracts information from documents like bills, prescriptions, and discharge summaries using AI-led classification. It also flags mismatches against policy terms and can detect potential fraud, significantly reducing the administrative burden on HR teams and Insurers. Claims are submitted via familiar channels like Mobile App, email or WhatsApp, with real-time alerts for missing or invalid documents, cutting delays before they begin.
Powered by AI, OCR, and NLP, ClaimSetu: Automates document reading from claim forms, pharmacy bills, hospital bills, prescriptions, discharge summaries, etc.
Flags missing or incorrect documents in real-time Provides employees with claim insights approval based on Policybazaar’s vast historical claims data and constant updates at each step of the claim process.
Intelligent claim routing: Assigns claims to appropriate teams based on document completeness, complexity and assistance estimated.
Secure, Scalable, and Future-Ready ClaimSetu is built with strict adherence to data protection norms, ensuring enterprise-grade security. The platform is also designed to integrate seamlessly with Customer Relationship Management (CRM) systems, Insurer backend systems, and HR tools.
In its beta version, while it currently supports GHI reimbursement workflows, ClaimSetu’s modular architecture allows for expansion into OPD claims and other categories in the future — making it a future-ready engine for insurance operations across different product lines.
By eliminating manual work, reducing turnaround time, and creating a more empathetic claims experience, ClaimSetu is poised to set a new benchmark for enterprise claims handling in India’s fast-changing workplace.
(Disclaimer: The above press release comes to you under an arrangement with PNN and PTI takes no editorial responsibility for the same.). PTI PWR PWR
AI-led claims processing compliance enhances group health insurance reimbursements, flagging policy mismatches and safeguarding data privacy. ClaimSetu is an AI-driven engine for Group Health Insurance reimbursements that automates document extraction and reading, provides quantitative claim scoring and approval insights, flags missing or incorrect documents and potential fraud in real time, routes claims based on completeness and complexity, offers live tracking and alerts, integrates with enterprise systems, and is built with asserted compliance to data protection norms and a modular, scalable architecture.
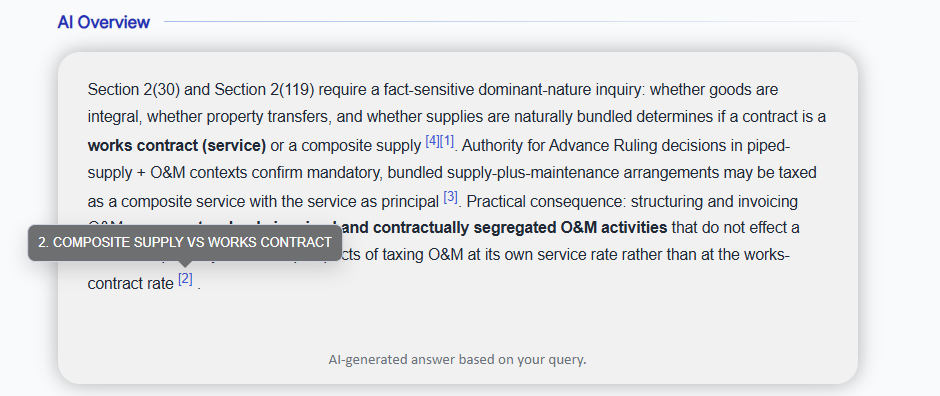 • Category-wise results to explore all relevant documents on TaxTMI
• Category-wise results to explore all relevant documents on TaxTMI
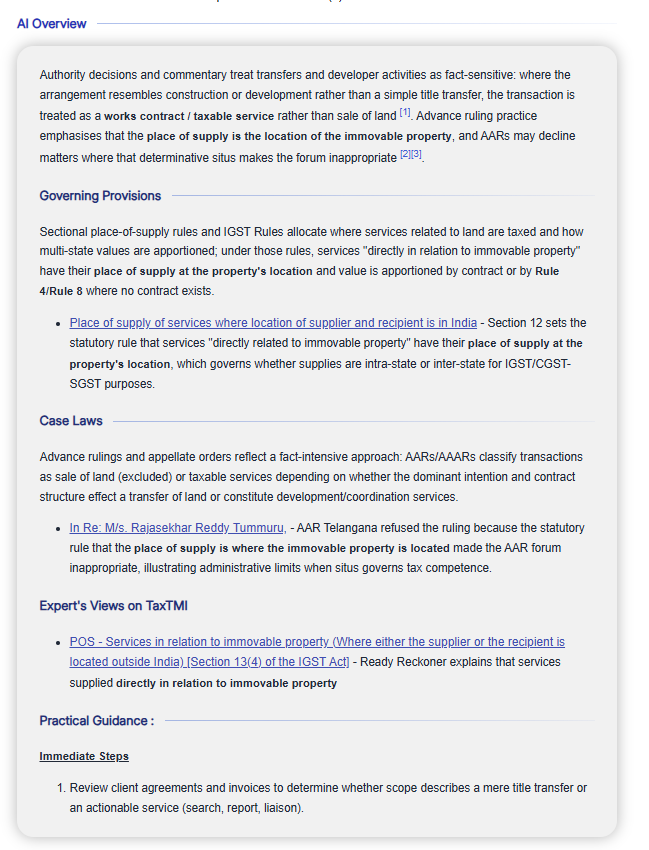 Help Us Improve - by giving the rating with each AI Result:
Help Us Improve - by giving the rating with each AI Result:
 TaxTMI
TaxTMI  TaxTMI
TaxTMI